Client Welcome Letter,
I am excited about YOU going through the PLP (Passionate Life Program). May this be the change you are looking for in your life.
Many clients feel trapped when they finally agree to have counselling. PLP (Passionate Life Program) is not like standard counselling. Our counsellors are highly empathetic, and trained for complex mental health and/or addiction issues. The program has been created to empower clients, and transform their lives for the better. Even though the program has 6 or 12 steps (depending on which plan), the counsellor prioritises the client’s needs with every 1 x hour session. The process is structured, yet organic.
You may have social phobia or agoraphobia, from traumas you have experienced. You may have severe anxiety, depression, grief, or you may be using drugs, alcohol, or gaming, in an attempt to distract yourself from your emotions and life. You most likely don’t even like yourself at times. You may be socially isolated, or simply feel stuck/frozen in your life. Or you may have just had a bad run, and need some extra support/tools, to move ahead. In PLP, our counsellors listen, without judging. We know that change is possible, because we see it constantly. Giving you hope for an easier and better life, is what we do… and we also give you the tools to make this happen.
We empower you with a 3-point healing process:
- Identify and change problematic programs in your subconscious.
- Offer healing of traumas/blocks with somatic therapy (specialised trauma release).
- Provide simplified psychoeducation for you so you can understand and normalise symptoms. We help you understand what is happening in your brain and body, in relation to anxiety, depression, grief, and addiction.
Ultimately, our goal is to help you move forward in life, with strength, improved motivation and self esteem, and reduced (or recovery from) substance use.
The PLP program normally causes reduction in mental health symptoms, which often results in employment. PLP (Passionate Life Program) is a 6 or 12 week Telehealth Program created for clients with Self Esteem, Motivation, Depression, Anxiety, Grief or Addiction Issues.
The Employment Consultant creates the first appointment, and the client attends weekly, for one hour per week. Our counsellor will call you at the same time each week, and after the first appointment, a Telehealth link can be used, so you can see your counsellor. You will continue to work with the one counsellor you start with.
This program has been operating with many job agency clients throughout Australia with outstanding results!
______________________________________________________________________
Assessment:
All clients participate in a life balance wheel, which is an eight point psychosocial assessment on: Your thoughts, self-esteem, grief, emotional, management, physiological state, social networks, hobbies, and your daily lifestyle satisfaction. You will also be asked about any substance use or medication, as well as scanned for any potential traumas by being asked about any operations, life-death situations, or loss.
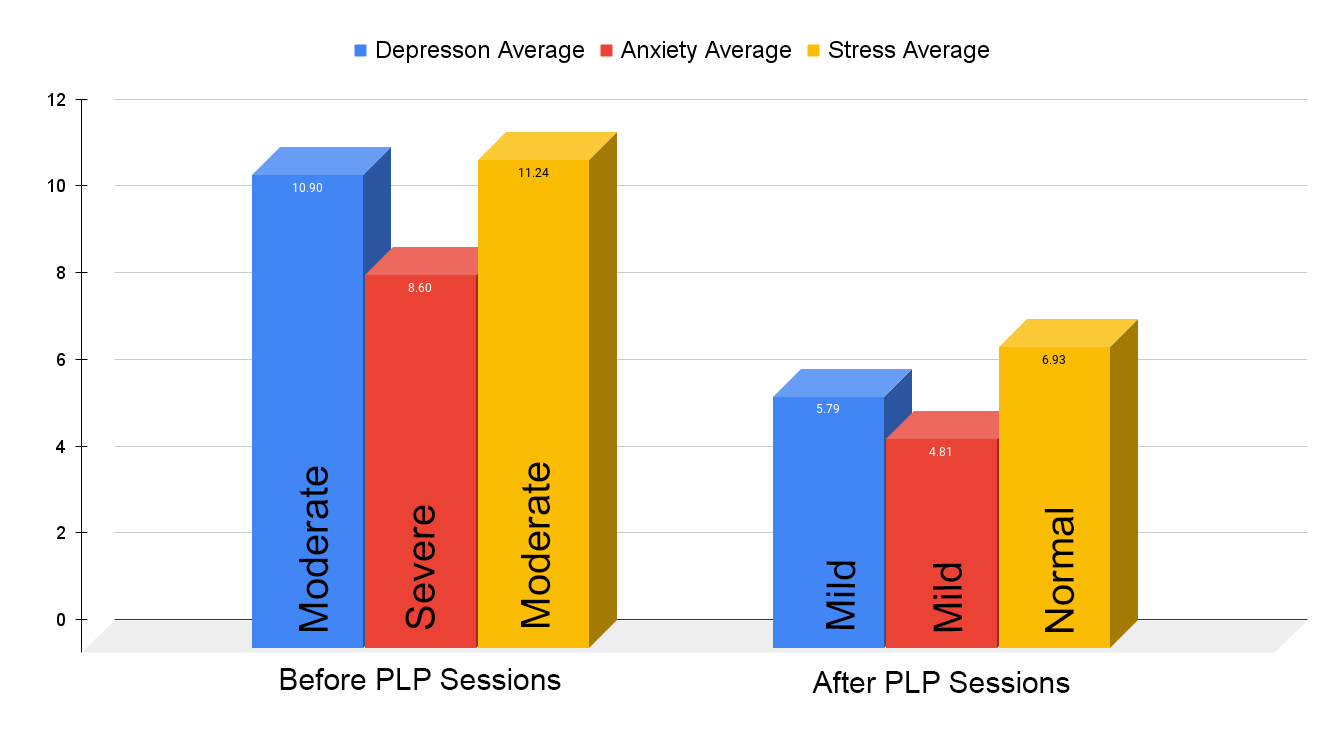
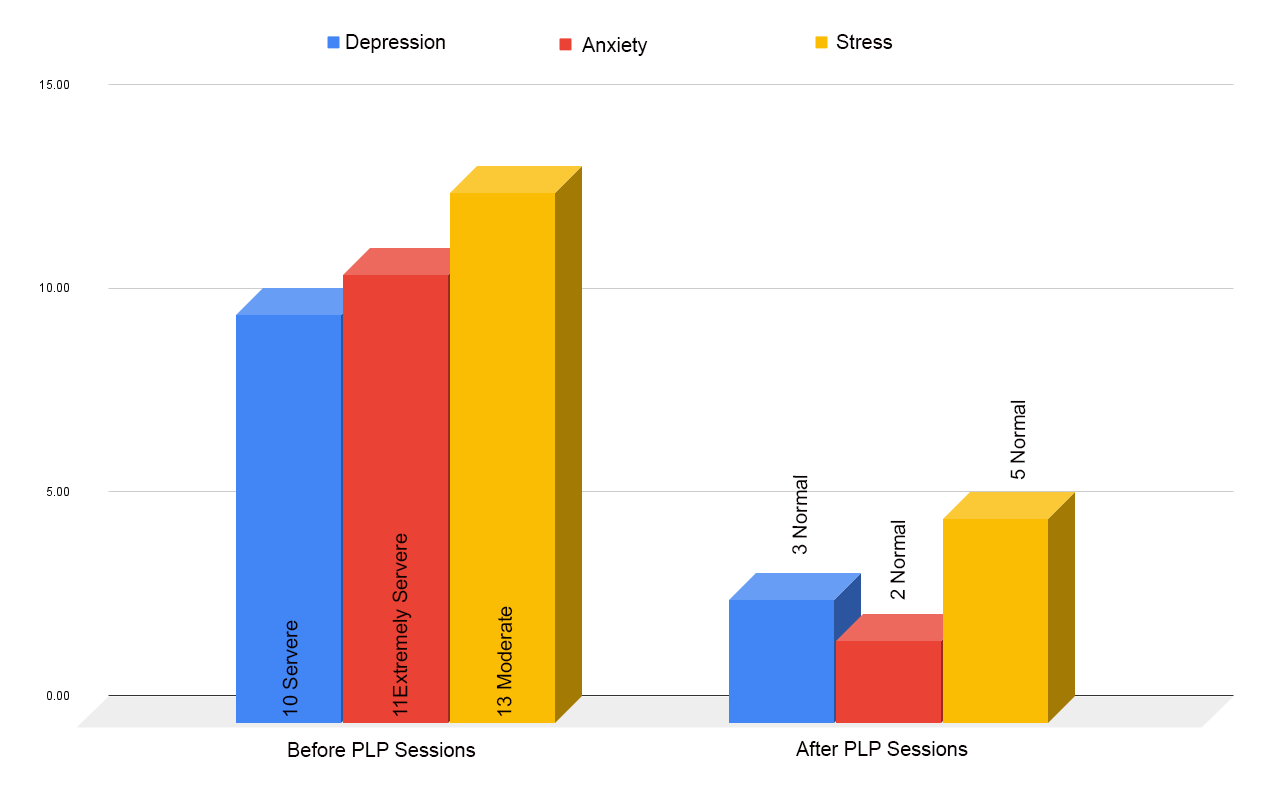
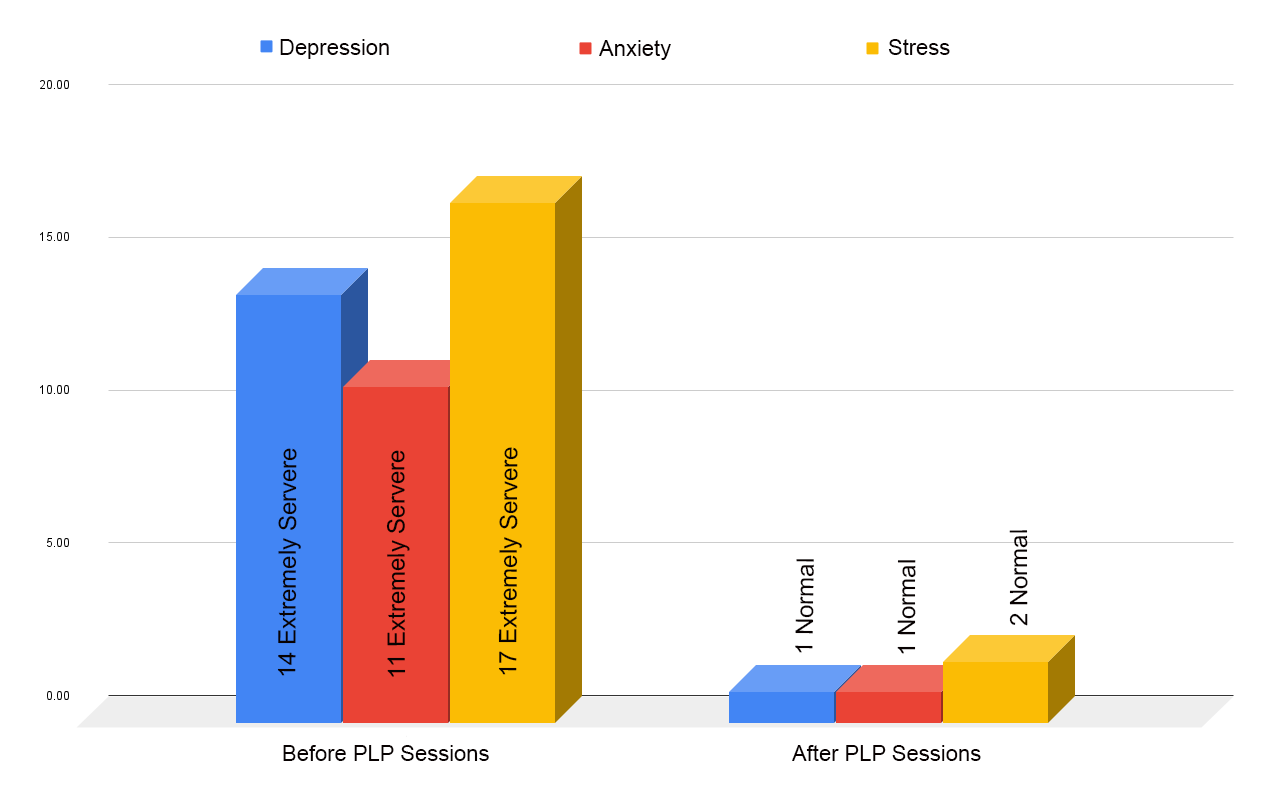
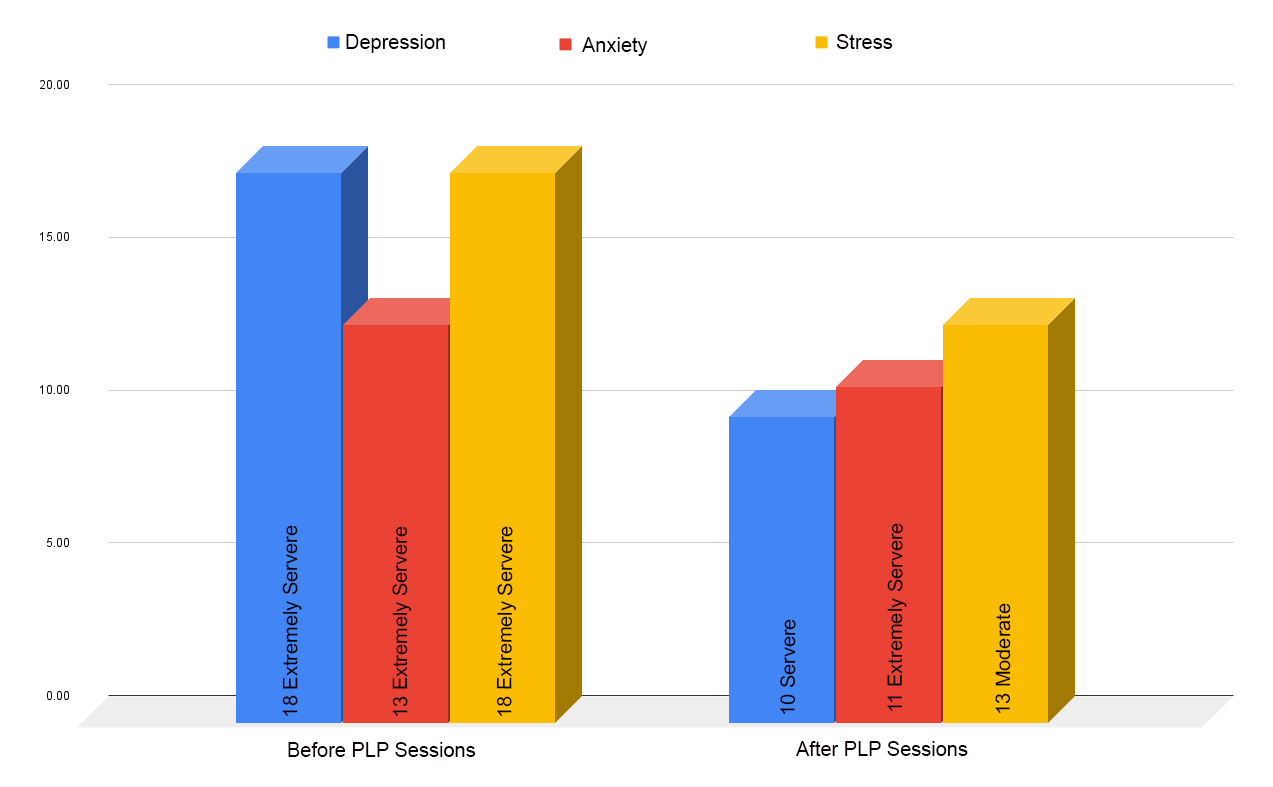
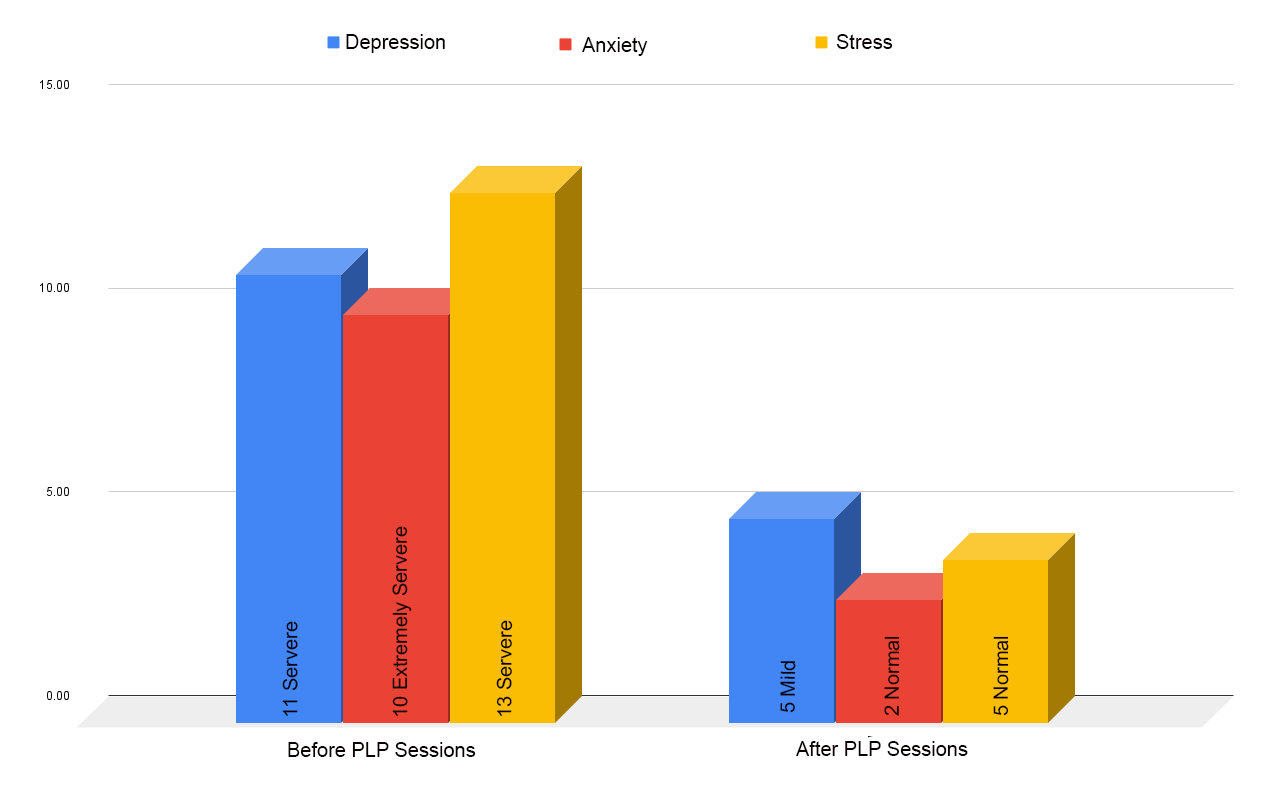
The PLP (Passionate Life Program) works through the life balance wheel, and DASS21 to gather progress reports. You will be encouraged at the end to do a feedback form, which also outlines changes you have experienced throughout the program.
At PLP, we believe that when working with addiction, the first area that needs to be addressed are the contributing factors (anxiety, depression, and grief). We then equip the client with psychoeducation in these areas, do trauma release (somatic therapy), help clients understand patterns in the subconscious, and then get to work on addiction strategies, if addiction is present.
Throughout the program, you are given options for strategies for whatever you may need support with, such as: anger management, relationships, parenting, simple education on neural pathways, brain activity, brain chemistry, reward pathways, neural networks, and personality. You are given tools to be able to collate many tools together in our task sheet. Clients can proactively utilise the tools and move forward in your life. You will always be encouraged to discuss the issues they are having that week, as our program is dedicated to you.
We support you. You may need case management, letter of support, external referrals, letters to centrelink, or much more.
You, the client, always comes first. Most important of all is that you want to change, and participate in this program. Our role is to treat you with high empathy and respect, as we work together on a better life.
The PLP (Passionate Life Program) has been a development for 10 years, and has transformed the lives of thousands of clients in the decade. Since PLP Solutions started IN 2020, our team has helped many clients in job agencies all over Australia.
Self-esteem building:
In PLP, self-esteem is looked at as being the absolute cornerstone of improving your motivation and your relationships. From the very first session, your counsellor will begin to work with you to create a healthier self-esteem. Our counsellors are trained to energetically love all our clients, to identify strengths, and to work with you, so that you can discover more of your strengths.
When you have great Self Esteem, you become unstoppable. Great self esteem is a must for great relationships, high motivation, and more. If you care about you, you are more likely to reduce your addictions, and work harder at having a better life. When you don’t like yourself, you are more likely to abuse yourself, as well as tolerate abuse from others.
Trauma and your brain:
Whether it is childhood trauma, one or multiple traumas, the result could have an impact on your brain, body, nervous system, and your life. Think back to any life/death event you have experienced, such as a loved one needing an ambulance urgently.
Your Brain: In that moment, the practical part of your brain takes over. You talk to the ambulance, help comfort your friend/loved one, but the screams of: ‘Oh my God! You nearly died!’ remain unprocessed in the subcortical part of your brain. (The part of your brain where your emotions are processed, but there are no words.)
This unprocessed emotion can trigger your Vagus nerve for months, or years, to come.
Your hippocampus normally files your emotional memories as the past, in your brain. However, during a traumatic event, your hippocampus becomes flooded with cortisol, the stress hormone, which affects its functioning. This means the memories of a trauma may not have been filed away, and can feel as though the trauma has just happened… even months or years later.
Talk therapy can only do so much!
Somatic therapies such EMDR (Eye Movement Desensitisation Reprocessing) can assist in the processing (the filing) of these emotions in the brain, which has been shown to reduce anxiety and PTSD symptoms.
Your Nervous system:
The Autonomic nervous system has two sides. Parasympathetic and sympathetic. Parasympathetic (rest and digest), is the calm side of the nervous system, and sympathetic (fight, flight and freeze), is the active part of the nervous system. If you’ve had a lot of trauma, or even one serious traumatic event, the trauma could cause PTSD (Post Traumatic Stress Disorder), and you could find that you are unconsciously flipping into fight and flight (sympathetic nervous system) often. This could lead to anger outbursts, a feeling of sickness in your stomach, heaviness in your chest, or you could feel (or become) sick or unwell.
You could also find that you are dissociating, which means that you are not focusing, not present, feeling a type of brain fog, as the brain constantly puts you in a freeze-like state.
Trauma Symptoms:
Flashbacks (intrusive thoughts about the traumatic event), Nightmares, Avoidance behaviour (agoraphobia or social phobia), Anger outbursts, Hypervigilance, Shaky legs, Insomnia, Trouble concentrating, Obsessional thoughts about the trauma, Rapid speech, High blood pressure, Sweating, Feeling sick in the stomach or heavy in the chest (often).
Examples of Traumatic Experiences:
House Fire, War, Car accident, Being robbed, Operation, Watching a loved one die, Hearing horrific details of a trauma (vicarious trauma), Sexual Assault, Losing custody of your children, Violent altercation or witnessing violence.
Anxiety is a chronic situation.
It is often the result of one traumatic experience (being robbed), or many traumatic experiences (Childhood trauma or a long term abusive relationship). Anxiety can also be from constant negative thoughts, a lifestyle that is stressful, or addiction.
Anxiety is different from stress.
With stress, you may find that you feel nervous, your blood pressure changes, your heart rate increases or you may even get a dry mouth. Once the incident (or the stress) is over, you go back to normal state, physiologically and psychologically. At any given point in time, your level of stress in your body should feel like 0 to 1 (out of 10). If you have anxiety, you could find, on a day-to-day basis, you feel that your body is 4 out of 10, if 10/10, in the worst possible feeling. Anxiety is a crisis that affects millions of people. It can be managed and symptoms can be reduced. PLP can help!
There can be a physiological base to anxiety. You may need to go to the doctors and have blood tests, as your health may need to be investigated. Commonly, anxiety is from our patterns of behaviour, and/or our thought patterns, that keep us trapped in a world of ingrained distress.
Anxiety Symptoms:
Hypervigilance, Easily distracted, Feeling heavy in the chest, Feeling sick in the stomach, Diarrhoea, Heartburn, Sweating excessively, Panic attacks, Avoidance behaviour (Agoraphobia or Social phobia), Anger outbursts, Restless legs, Insomnia, Trouble concentrating or Mood swings.
Causes of Anxiety:
Childhood trauma, Addiction, Mental or physical illness, Physical or emotional abuse, Past Incest or sexual abuse, Being bullied (past or current), Burnout, Health issues such as hypothyroidism, Chronic negative thinking, Traumatic event (Being robbed, assaulted, loss of job, loss of belongings in fire or theft, loss of loved one/friend/financial status, or car accident).
Agoraphobia and Social Phobia:
Sometimes you need professional help to work through your grief. In some cases, you can have a ‘trauma grief’, which is serious. You may have experienced the death of a loved one, witnessed an accident, and combining grief and trauma can cause your emotions to be suppressed in the subcortical part of the brain. You could find that you are not able to move forward in life… you feel stuck. This is very normal in some very abnormal situations. You may have been through a traumatic loss, lost your job, and still be working through all the negative emotions. Your brain (subconscious) may not feel safe, as what you have been through was profoundly traumatic. Your brain tries to protect you from more trauma, so you begin to feel like even going to the supermarket is unsafe…or being around people. You could end up with Social Phobia or Agoraphobia, from a traumatic event…even if this event lasted only minutes. Having social phobia or agoraphobia, feeling like you cannot move forward, is a crippling state!
In PLP, we search for this type of trauma, then we use therapeutic tools to help your brain feel safe again. Once you feel safe, you will no longer feel stuck. We have helped many clients who previously felt frozen by PTSD, Social Phobia or Agoraphobia, heal and live a normal life again.
Depression:
Depression often stems from not feeling connected to life, or feeling a lack of purpose.
When you feel oppressed in your life (when you feel powerless) for a long enough time, you are very likely to get depression.
Depression is an imbalance of brain chemistry, and it’s often due to habitual thought patterns and action (or lack of action). If you feel that you have depression, while you need to see a doctor, you also need to become powerful in your life. PLP can help with specific tools to help you connect to your life again. Depression does not have to be permanent. PLP has transformed many people from depression.
Depression Symptoms:
Insomnia, Fatigue, Appetite changes, Negative thoughts, Reduced motivation, Increased anger at self.
Grief
Grief is a physical and psychological process over loss. It may be the loss of a friend, loved one, job, status, or any time when you feel like you have lost something… even the loss of a beloved pet. Grief usually causes a physiological change in your body and dramatically impacts your mental health. You may find it hard to concentrate, have fatigue, or a reduced appetite. Grief is a normal process, however, it is when grief is complex, problems usually arise. Grief can be complex due to many factors. Complex grief may be: suppressed, delayed, or chronic grief.
Examples of Complex Grief:
Suppressed Grief: You have to plan the funeral, and ensure all your siblings are ok, so you shove emotions down deep, and use excess alcohol to distract yourself for months.
Chronic Grief: Your favourite grandmother dies, you lost your job, and your mother is very sick, and in hospital. You have not processed your grandmother’s death, and you feel overwhelmed by grief, and are very impacted.
Delayed Grief: Your step dad has passed away, and there is a delay in the funeral. Finally you attend the funeral, but you are so busy making a living to support the family, that you never feel you had a chance to feel this loss. Over a year later, you break down, and cry for an hour, and feel the enormity of your loss.
Grief is like a train going through a tunnel. Over time, you will see little glimpses of blue sky from your Grief Tunnel. Eventually, you will come out of the tunnel, and see all of the blue sky again. Life is meant to return to normal again…it just doesn’t feel like it will, at the time.
However, when you are suffering from complicated grief, and not facing your loss head on, you may find yourself turning to addiction to try and numb these challenging emotions, and to shut out the pain.
In PLP, we help with the grief process, by offering somatic therapy and trauma release to help you process the loss, and we give you tools to be able to help with the grief process. We give you strategies to show you how to move forward in life and normalise your loss.
Grief Symptoms:
Trouble concentrating, Appetite changes, Fatigue, Reduced motivation, Sadness, Anger
Numbness, Denial, Bargaining (Why wasn’t it me?).
Relationship Tools:
Our brain is the most important Real Estate in the world. What you think about, every second of the day, determines what you get out of life. If you are in a toxic relationship, you can become obsessive about what the other person said, did, and STOP focusing entirely on your own life.
In PLP, we search for signs of abuse and control. If we spot abuse signs, we educate and heal the client. You can focus entirely on your life, and not be distracted by many negative emotions, if you have healthy relationships. In PLP, we teach clients who need help, how to have better boundaries, as well as improved, loving, and healthy relationships.
Thought Transformational Tools:
Regardless of what happens to you in your life, you can change your thoughts. However, you need to start with understanding what your problematic programs are in your subconscious (about your life and yourself).
In PLP, we identify your problematic subconscious programs, so that you can change these problematic programs. What do we know about our subconscious programs? They cause your automatic thoughts, which impacts your thinking every day. Our PLP counsellors teach you how to change some of these programs, how to start to understand your thoughts so you can change them. Some CBT (Cognitive Behaviour Therapy) is used here, but also other techniques.
Goal Setting:
The PLP has a number of tools to enable you to understand the ways in which you can achieve your goals. There is a work history exercise, which enables you to be guided through past work jobs; what you liked, what you didn’t like, and what skills you acquired, to help you understand you own professional strengths. This tool quite often is the catalyst for clients, changing their expectations about themselves, and frequently clients start work after this exercise. There are other tools utilised in PLP to help you understand how powerful you are. There are many articles and handouts to show ways in which you can radically change your life.
As it is my goal to reduce worldwide depression, working with you makes me so happy 🙂
May your love for yourself, and your life, deepen more daily.
Changing Lives; That’s what we do.
Phoebe Hutchison
Founder PLP Solutions
www.plpsolutions.com.au
Phone: 1300 750 760